Jaw surgery or more technically called as Orthognathic surgery corrects misaligned jaws. It can treat conditions like TMJ disorders, malocclusion (“bad bites”) and obstructive sleep apnoea. It’s a complex process that requires a lot of downtime.
Corrective jaw surgery or Orthognathic surgery changes the structure of your jawbone and brings your upper and lower jaws into proper alignment. Misaligned jaws can negatively impact your bite and make eating and speaking more difficult.
Jaw surgery, when you’re a TMJ patient, isn’t a single event. It’s a two- to three-year process that combines surgery and Orthodontics. Specifics vary for everyone, but here are the basics:
- Orthodontic treatment prepares your teeth for jaw surgery.
- Jaw surgery aligns your upper and lower jaws.
- Continued orthodontic treatment helps your teeth move into and stay in their final positions.

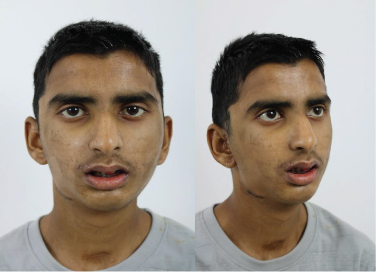
Why do TMJ patients need Orthognathic Surgery?
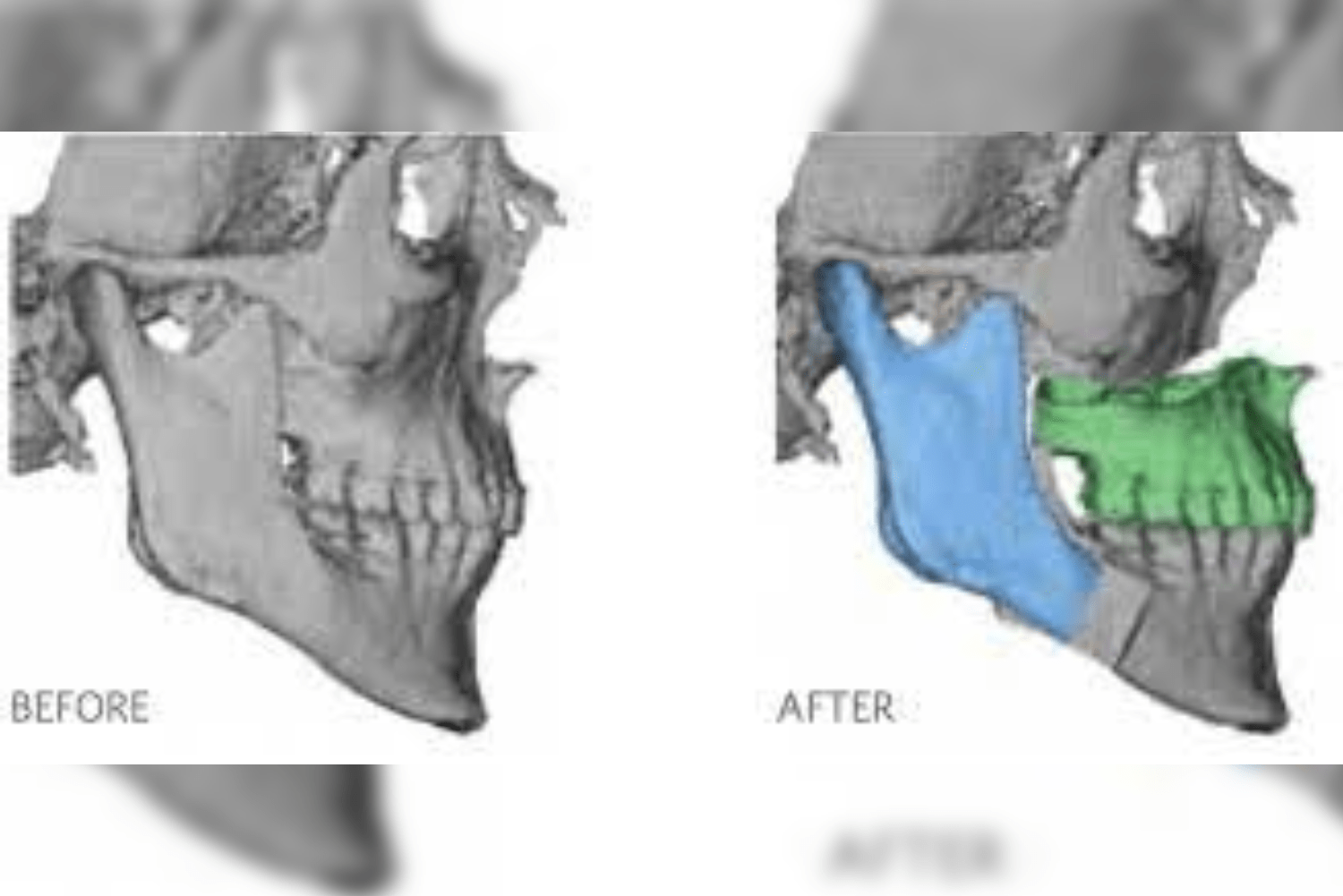
TMJ disorders often result in one side or at times, both sides of the lower Jaw to be unequal, asymmetrical and giving an obvious esthetic and functional compromise. Even after the ankylotic or disordered mass is surgically removed and reconstructed using a custom or stock implant, how the rest of the jaw grows is often unpredictable.
This results in an obvious dis-harmony not just between the two upper and lower jaws but also within the jaw itself. The resulting appearance of the patient is that of very obvious facial asymmetry and difficulty in mastication and speech.
The most common Orthognathic procedures that patients with TMJ disorders need are:
- Single or Bilateral Sagittal Split Osteotomy of the Mandible
- Differential Osteotomy of the Mandible
- Maxilla advancement
- Maxillary setback
- Genioplasty
At times, Distraction Osteogenesis may also be required along with the above-mentioned surgeries.
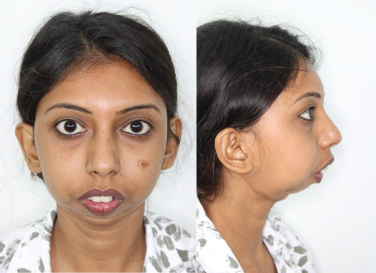

Which patients with TMJ disorders need Orthognathic Surgery?
Mostly, all patients who have TMJ disorders which affect their jaw mobility, shape and/or form require Orthognathic surgery. The following patients most definitely are in need of Orthognathic surgeries:
- Patients having TMJ ankylosis- Be it adults or children, once the ankylotic mass is removed, Orthognathic Surgery is needed to compensate for the asymmetric growth and position of the Mandible
- Patients who have had Condylar fractures during their growing ages, as a result of which, the lower jaw has grown disproportionately
- Patients having syndromes like Treacher Collin’s Syndrome, Williams-Beuren Syndrome, Ophthalmomandibulomelic Dysplasia
- Patients who have had infections in their TMJ or ears which have then resulted in fibrous or bony ankylosis
There are few patients who may need Orthognathic surgery but may be advised against it.
The following patients are contraindicated:
- Patients with a deficient bone form
- Local and/or inflammatory conditions around the tissues
- Those with a severe immunocompromised disease (pathology)
- Those with a very limited degree of achievable activity in their everyday life (bedridden patients, patients having mobility issues or patients with a disorder more severe than serious systemic disease)
Relative contraindications are as follows:
- Those with progressive or chronic inflammation related to their general condition
- Those compromised by systemic diseases, including immunodeficiency
- Patients in the period of skeletally immature growth
- Patients with obvious abnormal habits, such as clenching, grinding, etc.
- Patients who cannot understand and accept medical instructions after surgery (including those with neuropsychiatric disorders).
Planning of Orthognathic Surgeries in TMJ patients
Orthognathic surgery can either be planned traditionally using models or through modern digital methods like Virtual Surgical Planning
What is Virtual Surgical Planning (VSP)
Virtual Surgical Planning is a software modality using which digital planning and post-op result of the surgery can be planned and visualised. All the steps of the surgery can be computed here, including different ways of doing the same surgery, probable outcomes in all of these
Why VSP?
The traditional model surgery (TMS) used historically in orthognathic surgery planning is susceptible to compounded human and material error and leads to increased cost and time expenditures.
Virtual surgical planning (VSP) provides the ability to visualize surgical movements in 3D and has significant advantages compared TMS.
VSP has supplanted TMS as the standard of care in the treatment planning and execution of orthognathic surgery as new innovations continue to expand the potential to improve outcomes and increase efficiency.
VSP in Orthognathic Surgery
Using VSP, surgical movements are planned in 3D, allowing enhanced visualization of the anatomical changes induced by surgical movements. CAD/CAM technology allows for the fabrication of surgical guides in the form of occlusal splints or, more recently, custom patient-specific fixation.
Custom plates provide additional advantages including greater accuracy and improved surgical stability.
VSP in our Institution
In our patients with facial deformities, such as malocclusion, surgical planning and simulation of surgical outcomes are the most important processes in presurgical workups for successful orthognathic treatment. It is necessary to correctly move the osteotomized segment and dentition to the required position in 3D space according to the preoperatively determined surgical plan. Therefore, we believe in intraoperative control of precise and accurate mobilization of osseous segments.
Currently, we use NemoFAB software.It is the most comprehensive digital platform for orthognathic surgery. It’s an incredibly comprehensive tool for diagnosis and treatment planning for facial, airway and bite corrections. It uses Artificial Intelligence to recognize the teeth, maxilla, mandible and condyles in the CBCT achieving utmost accuracy and saving time. After planning the surgery, one is able to see the soft tissue morphing on the actual photographs of the patient’s face.
Pros and Cons of Orthognathic Surgery in TMJ patients
The advantages of undergoing Orthognathic surgery are numerous, all of which may probably not be possible to list out. Few of the pros are:
- It is the one final surgery that needs to be done to correct the asymmetry of the face which has resulted from TMJ disorders.
- It gives the patient a proper occlusion i.e. the correct bite of upper and lower teeth, which further aids in proper mastication
- It can be coupled with other surgical procedure, for example, if the TMJ prosthesis requires replacement or removal
- Distraction can be done along with Orthognathic surgery which results in new bone to be formed in the gaps in the jaws purposely inflicted by the surgeon to achieve symmetry
- It is the kind of surgery that achieves correction in all 3 planes
The disadvantages that come with these extensive surgeries are-
- Prolonged surgery time
- Prolonged healing and recovery time
- High cost
As with any other surgeries, Orthognathic surgeries also come with its fair share of complications.
No matter the meticulous planning and execution, some complications are unavoidable and are usually explained to the patients before surgery.
Conclusion
TMJ disorders are quite complex in the sense that even thought the joint per se is rectified and/or replaced, the resulting effect on the lower jaw and thereby its relationship with the upper jaw; and its resulting appearance on the face- all of this needs to be taken care of with the relevant surgeries. Patients having TMJ disorders have to be prepared for several surgeries that need to be done at various ages and stages of their life, out of which, Orthognathic surgery is the one that restores both form and function. Hence, it is a very important surgery and its timing and planning has to be meticulous.
Patients and their parents must be counselled at every step. Its only when the Surgeon, patients and their parents work in sync, desirable results can be achieved and the patient can be promised a life of proper form and function.