Does Diabetes Affect Ear?
Malignant otitis externa is a dangerous infection of the external ear that can also affect the middle and inner ear, skull base, and the temporal bone. It occurs in immunocompromised individuals, such as those with uncontrolled Type 2 diabetes. This highlights how diabetes affect ear and increase the risk of ear-related infections.
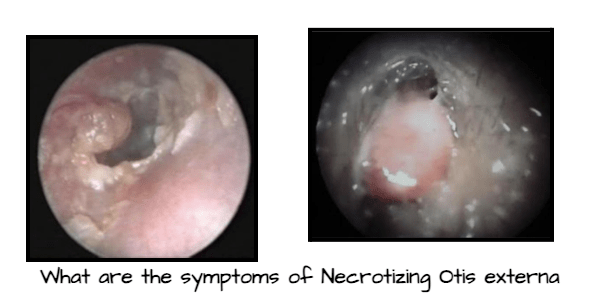
What are the Symptoms of Necrotizing Otitis Externa?
- High-grade fever
- Profuse purulent discharge in the ear
- Severe ear pain, especially at night
- Granulation tissue in the ear canal
- Severe itching
- Trouble swallowing
- Facial muscle weakness
- Neck pain and stiffness
Granulation in the external ear canal may also occur, which is more common in individuals with diabetes. Diabetes affect ear, increasing the risk of developing conditions like necrotizing otitis externa.
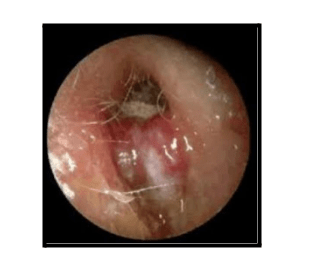
How Does Uncontrolled Diabetes Affect Ear?
Uncontrolled diabetes mellitus can cause small-vessel vasculopathy, which affects the small blood vessels and causes immune dysfunction. In patients with uncontrolled diabetes, the cerumen (earwax) in the ear canal has an elevated pH but reduced lysozyme levels compared to normal standards, making the ear more susceptible to infections. Diabetes affect ear by increasing the likelihood of infections such as necrotizing otitis media, which is caused by microorganisms like Pseudomonas aeruginosa, Klebsiella sp., and certain fungi like Aspergillus.
What Are the Complications of This Condition?
Necrotizing Otitis Externa (NOE) spreads through the fascial planes, causing erosion of bones and invasion of nearby tissues. This can lead to involvement of cranial nerves and the bones of the skull base. As a result, complications may manifest as facial weakness, hoarseness of voice, difficulty in swallowing, and tongue weakness. In later stages, the infection may spread to the brain parenchyma, leading to severe complications such as brain abscesses and seizures. Diabetes affect ear by increasing the risk of NOE, which can result in these potentially life-threatening complications.
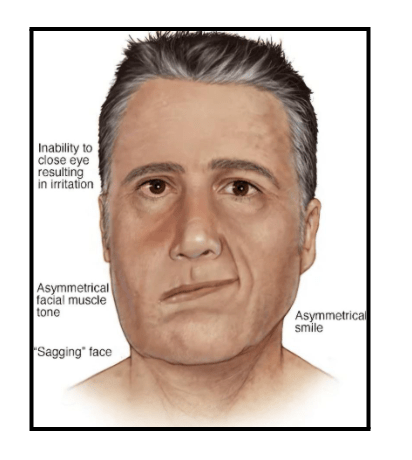
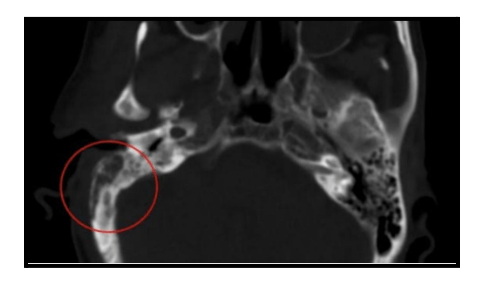
How Is It Diagnosed?
The diagnosis is primarily clinical, based on symptoms and signs, along with radiological findings from a CT scan. In cases where infection is suspected, a culture of pus (a sample of the discharge) from the ear or a biopsy of the granulation tissue from the external ear canal may be required. Diabetes affect ear by making individuals more susceptible to infections, such as Necrotizing Otitis Externa (NOE), which can complicate the diagnosis.
What Is The Treatment?
The main line of treatment is medical, which involves:
- Antibiotics, typically intravenously for the first few days, depending on the spread and extent of the disease.
- Corticosteroids, which may be topically applied.
- Strict and diligent control of blood sugar levels, which may require insulin therapy as diabetes affect the ear, increasing the risk of infections like Necrotizing Otitis Externa.
- Some individuals may require hyperbaric oxygen therapy, which speeds up the recovery process by promoting local healing.
Usually, Necrotizing Otitis Externa is treated with a 6-week course of antibiotics.
When to Approach Your Doctor?
It is advisable to approach your doctor whenever you have profuse ear discharge (foul-smelling), ear pain, or any symptoms associated with complications such as facial weakness, headache, ear pain, etc. Patients with diabetes should monitor their blood glucose levels frequently, along with their 3-month blood glucose levels (HbA1C), as diabetes affect the ear, making individuals more prone to ear infections.
At Richardson’s Face Hospital
At Richardson’s Face Hospital, we have the best team of ENT doctors who can provide prompt diagnosis and early treatment. Apart from early medical management, we also offer surgical facilities aimed at achieving a complete cure for advanced cases.